This blog has moved to a new website
Nutrition, Health & Wellness
Home ›
What is Marburg virus disease ›
What is leptospirosis - Leptospirosis in humans (Weil's disease).
What is leptospirosis?
Leptospirosis is a highly infectious zoonotic disease caused by the Leptospira bacteria affecting humans and animals. Icteric leptospirosis in humans is known as Weil's disease. It may also appear as an asymptomatic and subclinical infection. Leptospirosis symptoms range widely and are usually ignored or wrongly diagnosed as some other human sickness. Untreated infection can become icteric, leading to hepatitis, meningitis, renal failure, respiratory failure, pulmonary hemorrhage, and even loss of human life. The disease is more prevalent in tropical, subtropical and temperate climates.What causes leptospirosis?
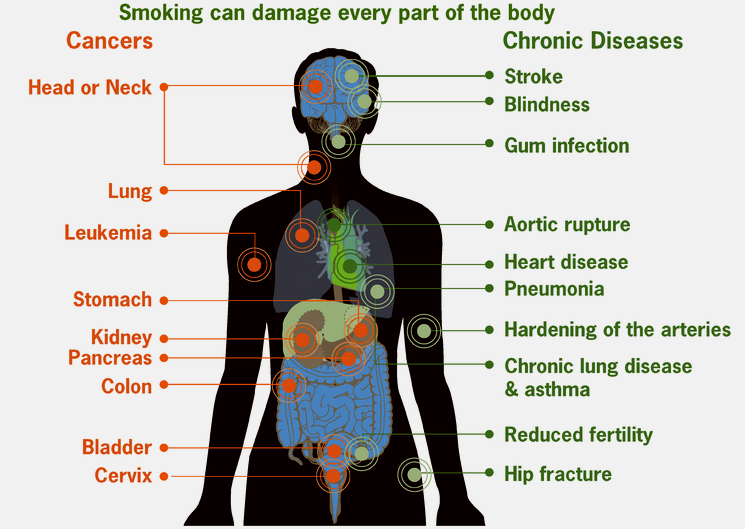
Leptospirosis is caused by the spirochetes (spiral bacteria). The spirochetes belong to the genus Leptospira, the family Leptospiraceae, and the order Spirochaetales. These anaerobic bacteria are thin, coiled and motile. Comprising several pathogenic and nonpathogenic species, typical disease manifestations in humans such as Weil disease, jaundice, pretibial erythematous rash, meningitis and gastroenteritis are associated with different serovars (strains). The bacteria can enter the human body through the contaminated water and food, skin injuries, animal bites and mucous membrane.| Popular topics: Signs and symptoms of pneumonia in children | What is Ebola virus disease | Diseases caused by smoking cigarettes | Baby teething fever | Baby teething rash on face |
The bacteria spread to humans through the urine, feces or body fluids of the infected animals. They can infect a wide variety of domestic as well as wild animals, which not showing any symptoms of the disease, may continue to shed the bacteria into the surroundings for months together. These infective discharges, by contaminating the drinking water and food, can spread the infection to humans and animals.
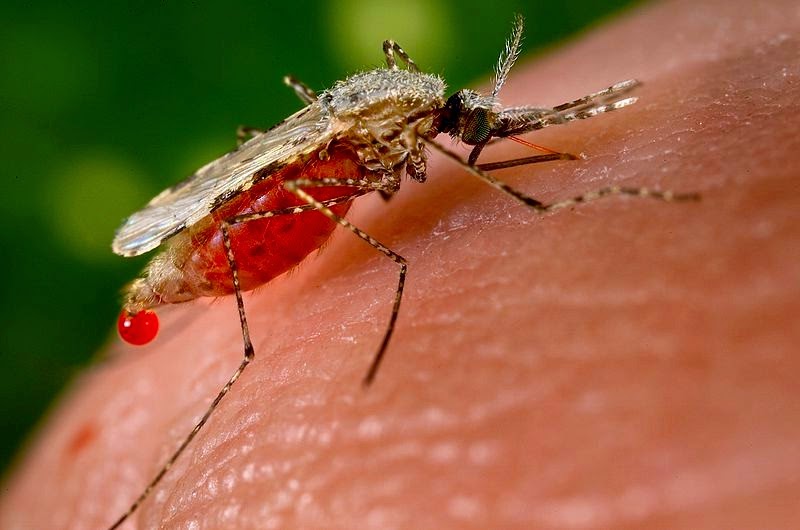
| Popular topics: What is malaria disease | Primary teeth | Neonatal teeth | Lysosomal storage disorders | Coping with dry skin in winter | Newborn tears | Syzygium aromaticum |
What are the risks of exposure?
Human occupational exposure to infected animals can also spread the bacterial disease among farmers, veterinarians, fish farmers, dairy workers, abattoir workers, sewer workers and animal caretakers. People associated with water sports like, swimming, kayaking, rafting run the high risk of contracting leptospirosis, if the waters are polluted.What are the symptoms of leptospirosis
The incubation period is usually 5-14 days but in some cases the symptoms have taken 2-30 days to develop in humans. The common clinical symptoms of the infection include, fever, headache, body pains, dry cough, rash, sore throat and chills. Gastrointestinal tract symptoms include anorexia, nausea, abdominal pain, vomiting, and diarrhea.| Popular topics: Baby teething age | Loneliness and health | Pneumonia in elderly people | Social anxiety depression | Chronic Sinusitis Treatments | What is high-fructose corn syrup |
Untreated leptospirosis may cause many systemic manifestations in humans, mostly by capillary vasculitis of the organ systems leading to hepatic failure, renal failure, pulmonary hemorrhage, respiratory failure, meningitis, interstitial myocarditis, adrenal hemorrhage, conjunctival suffusion and thrombotic thrombocytopenic purpura.
 |
| Leptospirosis causing bacteria Image courtesy: the Centers for Disease Control/Rob Weyant/public domain |
What is the treatment for leptospirosis
Mild infections in humans can be treated with doxycycline, ampicillin, penicillin, azithromycin, erythromycin or amoxicillin. For severe human leptospirosis, third-generation cephalosporins like cefotaxime and ceftriaxone may be administered. Intravenous penicillin G is also effective for mild to severe cases of infection.Related topics in health and fitness tips:
Pregnancy-related pelvic girdle pain.
Blocked tear ducts in newborn.
Horseradish roots.
Health benefits of celery juice.
Aspirin for cancer prevention.
What is Yo-yo effect.
Exercise and summer.
What is sleep hygiene.
Diesel engine exhaust causes cancer.
Loud music and hearing damage.
References:
1.Vijayachari P, Sugunan AP, Shriram AN. Leptospirosis: an emerging global public health problem. J Biosci. 2008 Nov;33(4):557-69.
2.Puliyath G, Singh S. Leptospirosis in pregnancy. Eur J Clin Microbiol Infect Dis. 2012 Oct;31(10):2491-6.
3.Wasiński B. Leptospirosis--current problems. Przegl Epidemiol. 2011;65(3):471-6.
Interesting topics in health and fitness tips:
Chronic low back pain.
Side effects of hypothyroidism.
Barley grass health benefits.
Magnetic Resonance Imaging uses.
Frequent headaches.
What causes sensitive teeth.
Amla fruit juice.
What is a soft drink.
Foods to control diabetes.
Peanut allergy in children.
Current topic in health and fitness tips: Leptospirosis in humans (Weil's disease).